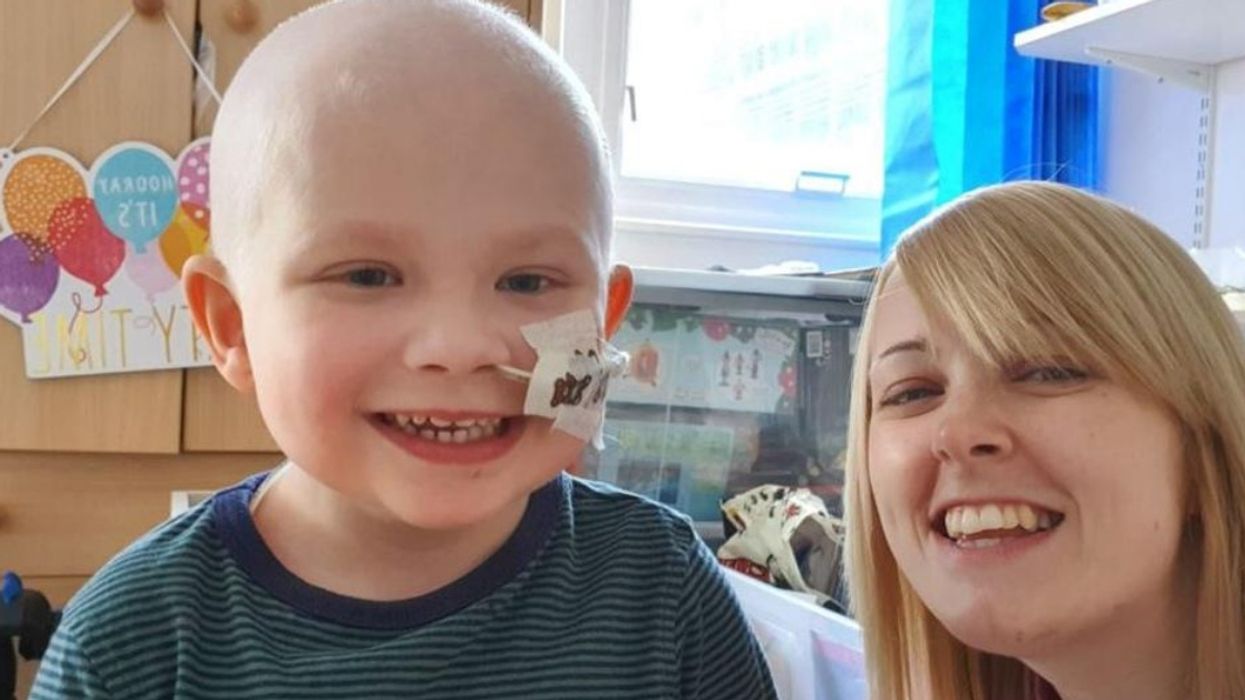
A devoted mom who believed a benign brain tumor had made her infertile told how the surprise baby she feared she would lose because of a rare genetic disorder is now living a normal life – thanks to a bone marrow transplant from a complete stranger.
Former clinical psychologist Zoe Alderson, 33, recalled how her joy was short-lived when Henry, the son she and her husband Craig, 40, a graphic design company manager, never expected to have was diagnosed with a rare genetic disorder, affecting just 125 people in the UK – meaning he needed monthly blood transfusions.
But everything changed in April 2019 when Henry – who has Diamond Blackfan Anaemia (DBA), which is caused by the bone marrow failing to produce red blood cells – received a successful bone marrow transplant.
Zoe, of Harwich, Essex, England, said he went from relying on transfusions to stay alive to having the blood count of a normal child his age, adding:
“We have no idea who provided the bone marrow, but not a day goes by when we don't think about that person. We will be forever in their debt."
“At one point, it felt like we would never have a normal life, now you can't tell Henry apart from any other happy four-year-old."
Zoe's own health problems began with fatigue, headaches and irregular periods throughout her teens.

But, in 2004, when she saw her doctor after her breasts began lactating, a blood test revealed she had higher than normal levels of the hormone prolactin. Amongst other things, it encourages the growth of breasts and lactation during pregnancy.
“I didn't have a clue what was wrong with me," she explained. “I wrote it off as being stressed and nothing more."
Referred to Colchester Hospital in Essex in November 2004, an MRI scan revealed she had a benign 1cm tumor on her pituitary gland, at the base of her brain and was put on a prolactin inhibitor – which she still takes to this day – and, within six months, the tumor shrank to 3mm.
“Doctors told me it was classed as a brain tumor, but I didn't need to panic," she continued. “They said I might face some difficulty getting pregnant, though."
“My periods were so irregular afterwards, that I never expected to conceive."
“I wasn't that bothered, either, as I was just happy to be told the tumor was benign."
Meeting Craig at a work Christmas do in December 2007, within a year they moved in together.
But, firmly on a career path, they flew to Mombasa, Kenya, for an intimate wedding with their nearest and dearest on March 17, 2010, and thoughts of having children could not have been further from their minds.
Zoe said:
“We really weren't fussed, or that's what we told ourselves."

She continued:
“We were both career driven and in our prime. We'd never even discussed the possibility of IVF or adoption – it just wasn't on the radar."
But all that changed in January 2015, when Zoe was plagued with morning sickness.
“I hadn't had a period for years," she said. “But I'd been sick for a solid few days."

She continued:
“At first, I dismissed it as a bug, but when it lasted over a week, I thought I should do a pregnancy test before I saw a doctor."
“I picked one up from the supermarket and when it came back positive, I just sat in the bathroom having a bit of a cry."
“It was such a shock, it was just crazy."
She continued:
“Craig was absolutely thrilled, though, for someone who had said he wasn't fussed about having a baby."
But soon Zoe was haunted by the feeling that “something wasn't right" with the pregnancy.
Then, at the 12-week scan, in early April 2015, the couple were told their baby showed signs of a genetic defect and was unlikely to survive to full-term, after finding a worrying amount of fluid around his head – which is often an indicator of chromosomal defects in a fetus, according to the NHS.
Zoe said:
“Craig, ever the optimist, was convinced we'd walk in and everything would be fine and dandy."
“But moments after finding the heartbeat, the woman's face dropped and before I knew it there were five medics huddled around the screen looking at the scan."
“We were asked to wait down the corridor where doctors explained there was a high chance the baby had a genetic defect and was unlikely to survive for two more weeks."
Given chorionic villus sampling (CVS) – a prenatal test to detect birth defects – after three days the results came back negative for the most common conditions, but further testing for rarer defects left the expectant parents playing an agonizing waiting game.
“It felt like we had already written off our baby at that point," said Zoe.
“We were carrying out the testing as an insurance policy, to see if there was a chance we could pass on any faulty genes in the future."
She continued:
“We were offered a termination but decided to let nature take its course."
And nature clearly had a positive plan for their baby boy, who continued to grow at a healthy rate.
“We hit 14 weeks, then 20, then 24 and somehow we even made it to 36 weeks," Zoe said.
She continued:
“We still didn't have the results back from the genetic screening, but making it so far surprised everyone."
“The consultant was amazed, he said he'd never seen such a poorly fetus survive to this point."
But, just days after the milestone scan, Zoe could not feel the baby moving and rushed to Colchester Hospital, where a scan showed he was in distress.
Concerned, doctors performed an emergency C-section, delivering baby Henry on November 20, 2015.
“When Henry was born we didn't know what was wrong with him still," said Zoe.
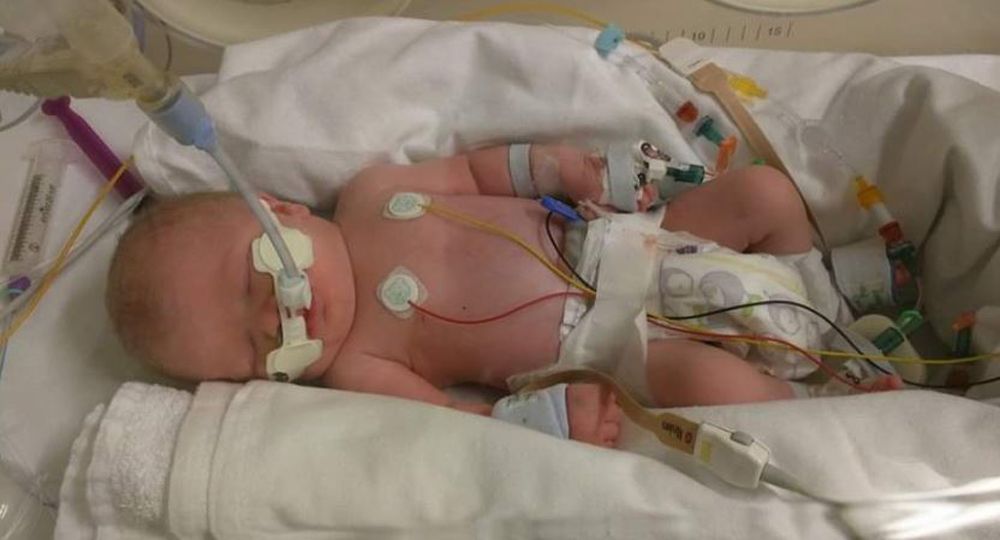
“He let out a cry, but was ghostly white and was rushed to neonatal intensive care."
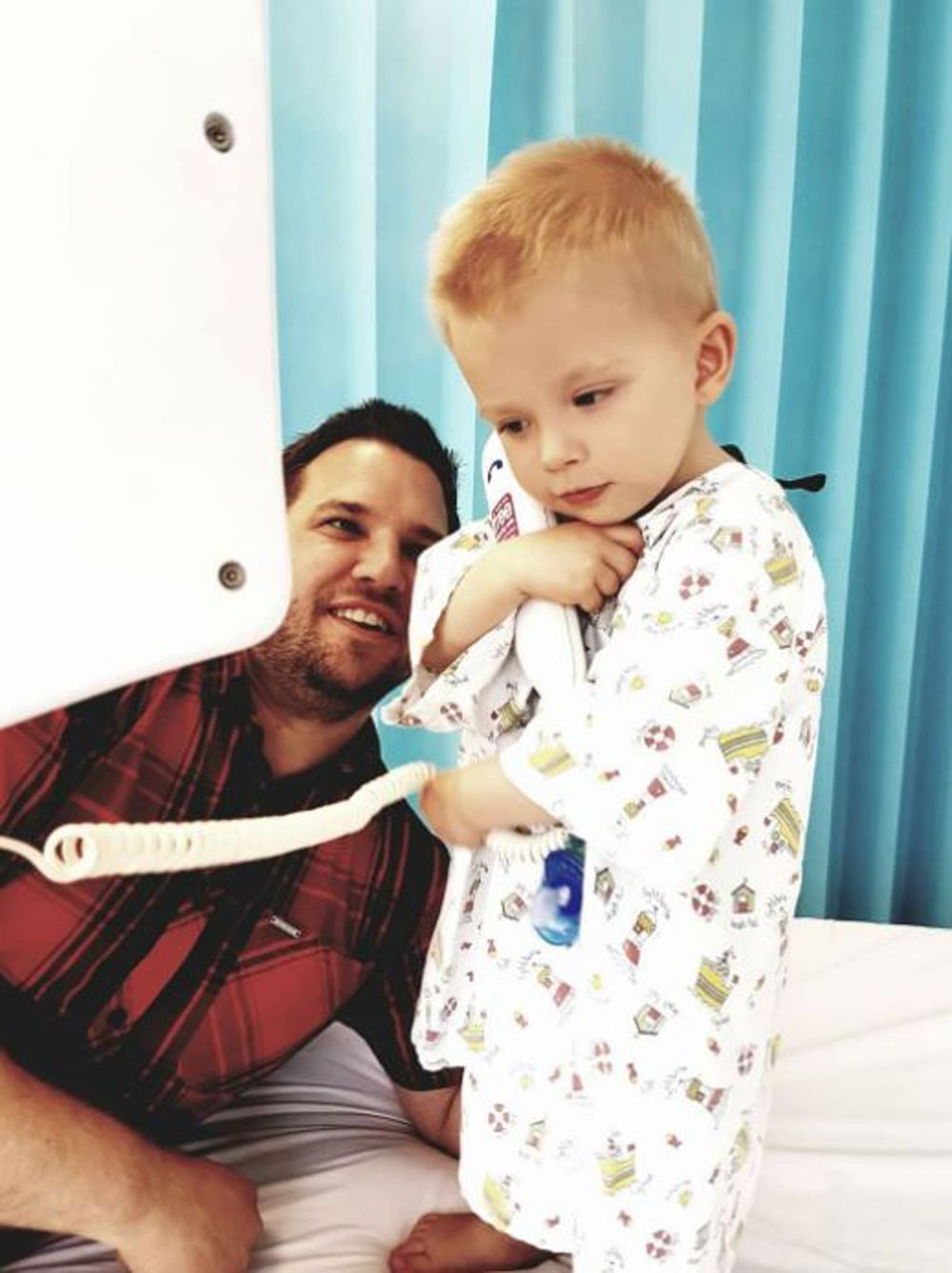
His pale complexion meant doctors assumed Henry had suffered from a placental hemorrhage in the womb, with a blood test showing he had a low red blood cell count.
Placed in an induced coma, the tot spent three weeks in intensive care, receiving three blood transfusions, to build up his red blood count.
“I didn't get to see him on the day he was born," Zoe recalled. “But I sent Craig down right away to keep an eye on him."
She continued:
“After the blood transfusions, he looked like a proper baby again and I couldn't wait to get him home."
Discharged at the beginning of December, the new parents were told to bring Henry in at the first sign of anything unusual.
He screamed “around the clock" and would not take to the bottle, but it was only when Henry turned deathly pale, on Christmas Eve, that the couple rushed him back to the hospital, where further tests revealed his red blood cell count was dangerously low – leading to another transfusion.
For the next three months, every month, the couple would return to the hospital for Henry to receive a blood transfusion until, at four months old, he had a bone marrow biopsy.
“Up until that point, all they could tell us was that Henry was anemic, but that they didn't know why," Zoe explained.
“The consultant examined the biopsy straight away and said it looked like he had DBA."
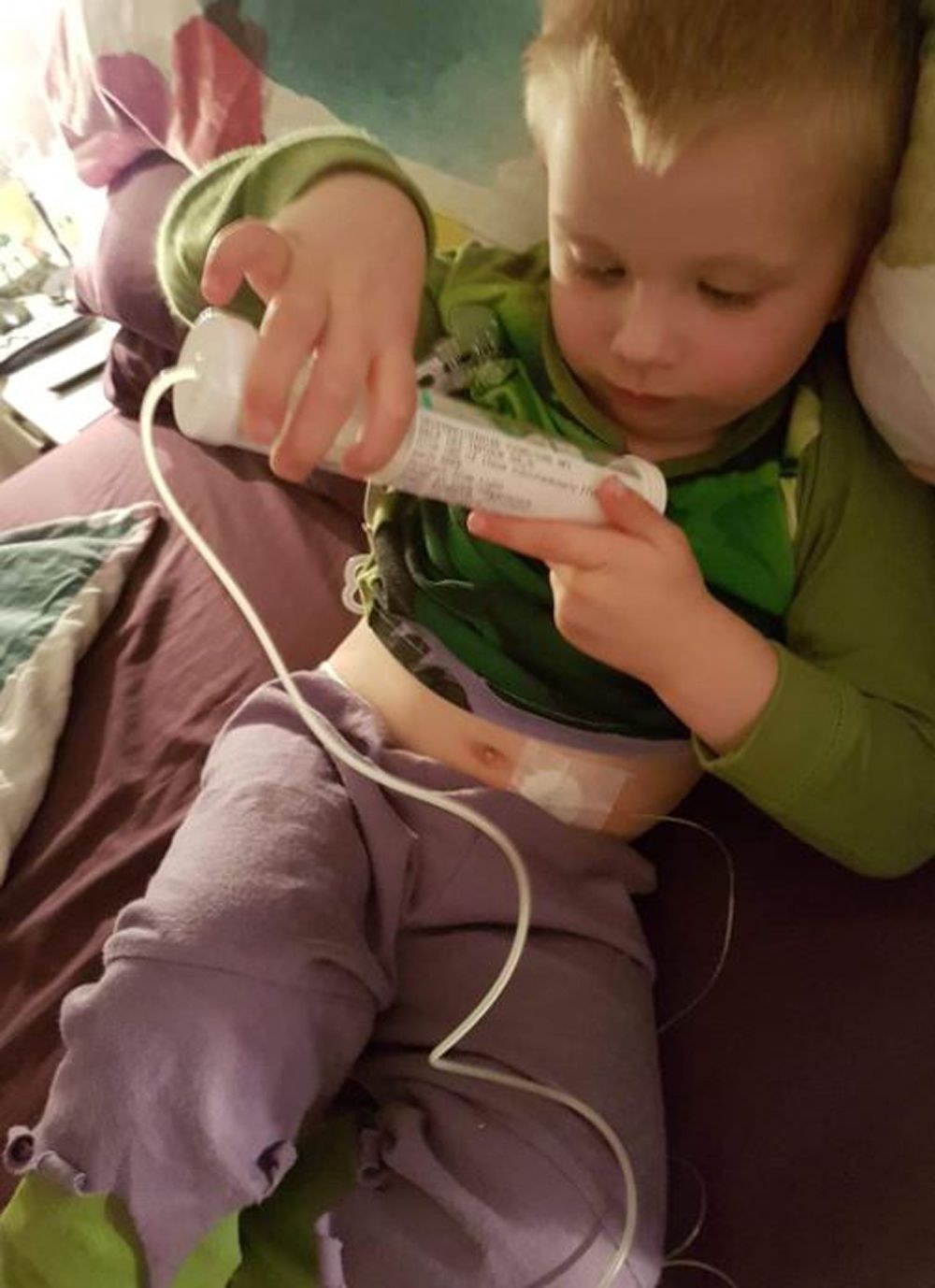
She continued:
“It was the first time we'd heard of it, but as soon as we got home and Googled it, we'd basically diagnosed Henry ourselves."
Two months later, by then six months old, his CVS results made the diagnosis official.
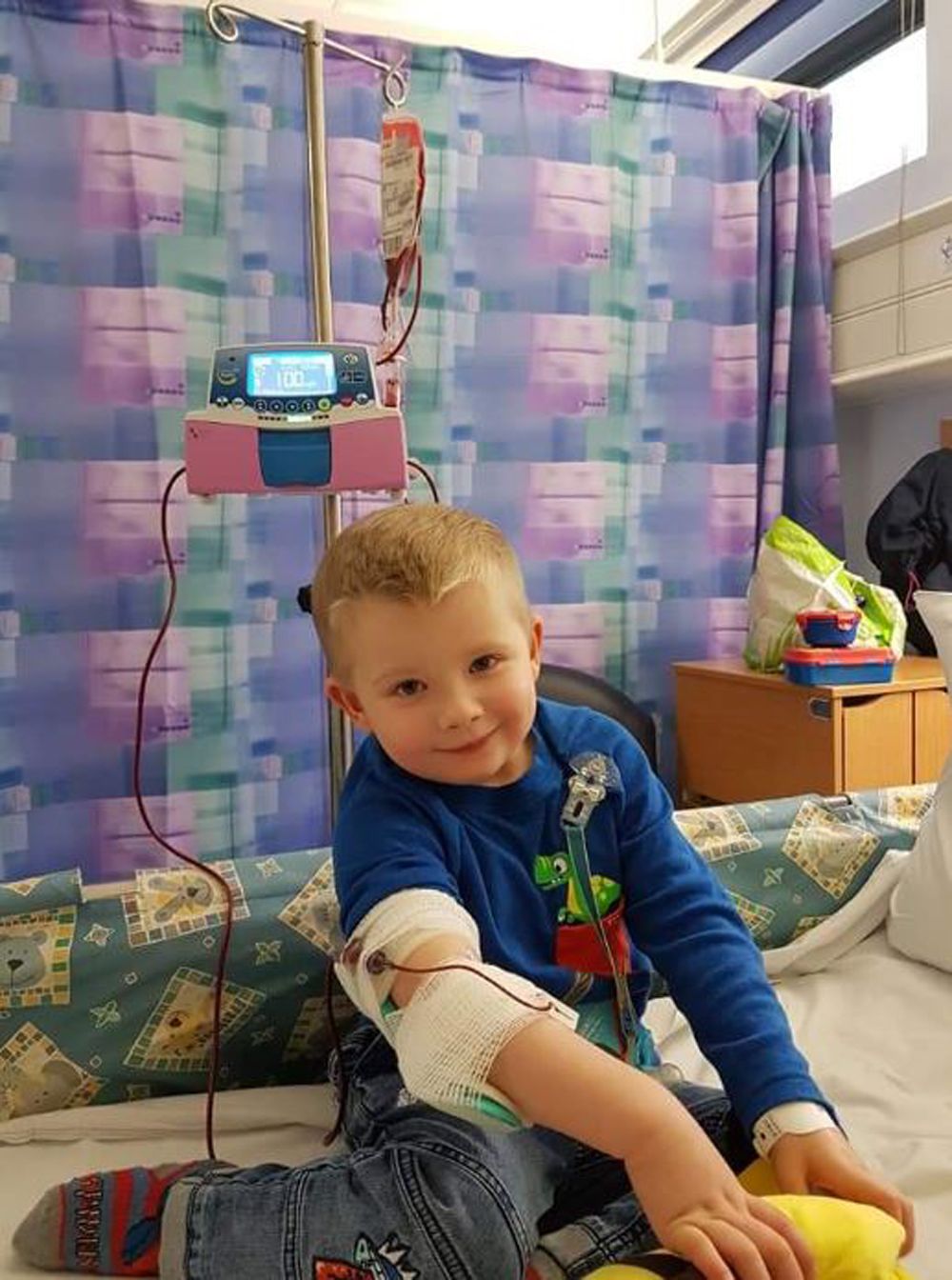
And, from then onwards, little Henry needed a blood transfusion every month – with doctors telling his parents this would continue for the rest of his life.
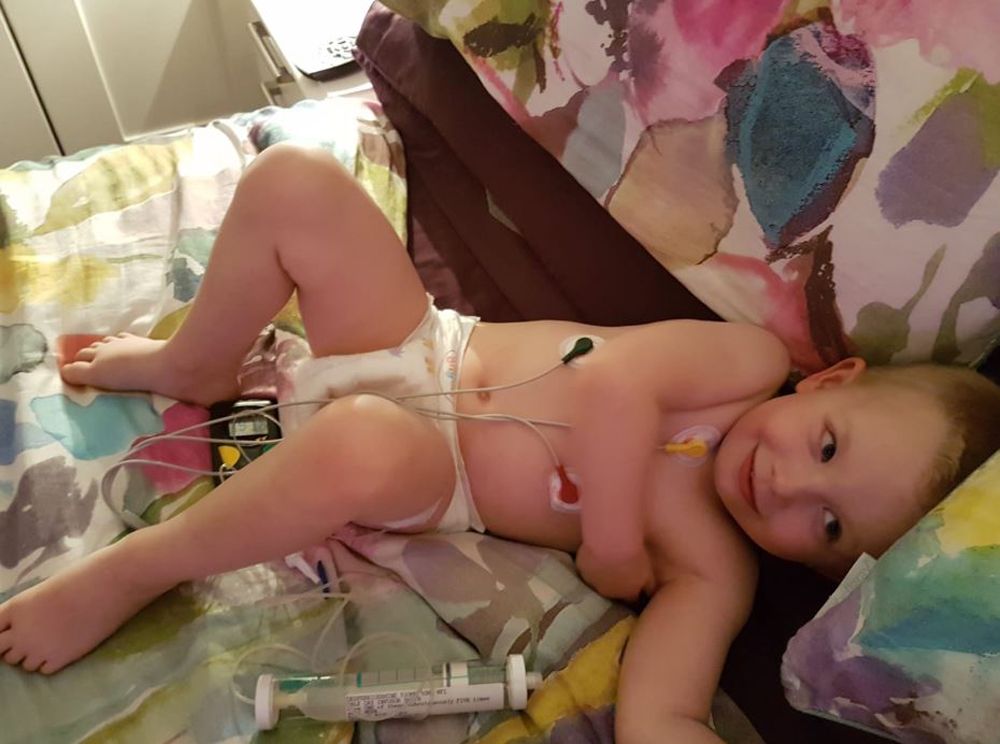
Zoe said:
“It felt like Groundhog Day. After the transfusion he'd be full of energy and behaving like a normal child."
“But slowly, as the days passed, you could literally see the life draining out of him."
“It sounds awful, but by the end of the month he really did look dead."
When he reach 18 months old, the couple were told Henry's body was suffering from an “iron overload," because of his numerous blood transfusions.
To avoid iron poisoning – which can cause severe damage to major organs – he began taking iron chelation drugs, to remove the excess mineral from his body.
Administered through an IV, which Henry was hooked up to every night, Zoe said:
“It was such a difficult period for us."
She continued:
“It was bad enough seeing him deteriorate each week, without having to start sticking a needle into him every night as well."
“He hated it at the time, but was fine during the day. Looking back, he was remarkably brave."
But when Zoe was told in February 2019 that he would need to be hooked up to the iron chelation machine 24 hours a day, she put her foot down.
“That's when I drew the line," she said. “It wasn't fair expecting that of a child and I said I wanted them to look into alternatives."
“That's when doctors said Henry would be eligible for a bone marrow transplant."
After that, by then aged three, things moved quickly and, just six weeks later, Henry was matched with a tissue donor.
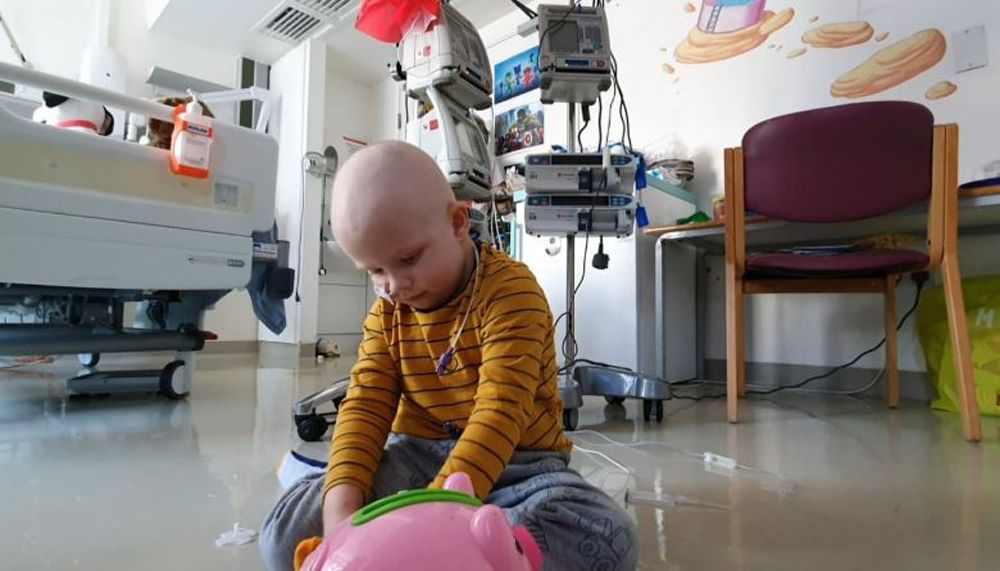
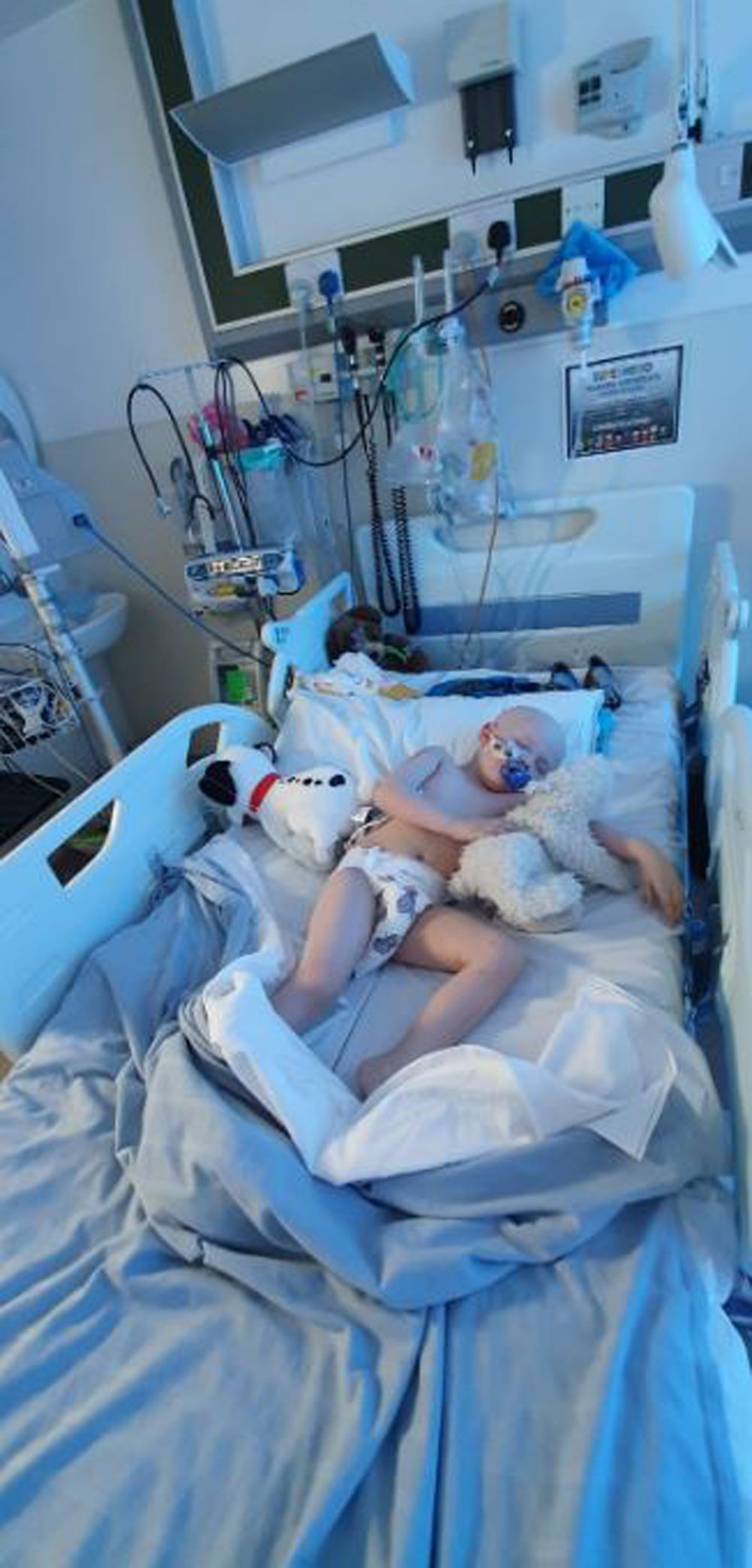
Then, in the last week of April 2019, he had chemotherapy to “wipe out" his existing bone marrow, before having a central line fitted, allowing the new stem cells to pass through his blood stream.
Put on immunosuppressants – a type of medicine which stop the body from rejecting donor tissue – for 12 months, Zoe said she witnessed a miracle, as she slowly got her boy back.
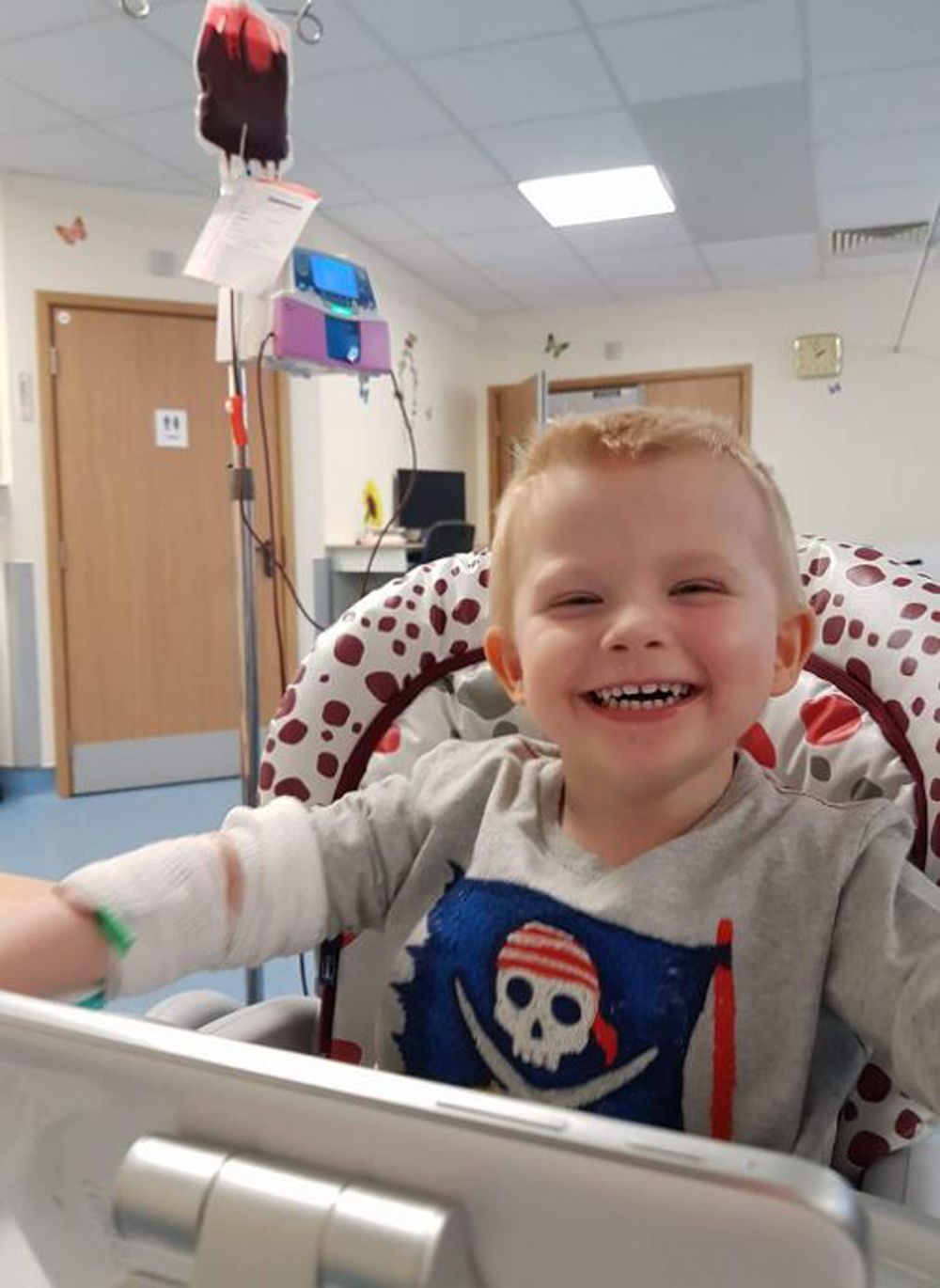
“He hasn't needed a blood transfusion since he had the bone marrow donation," she said. “He's a completely different child."
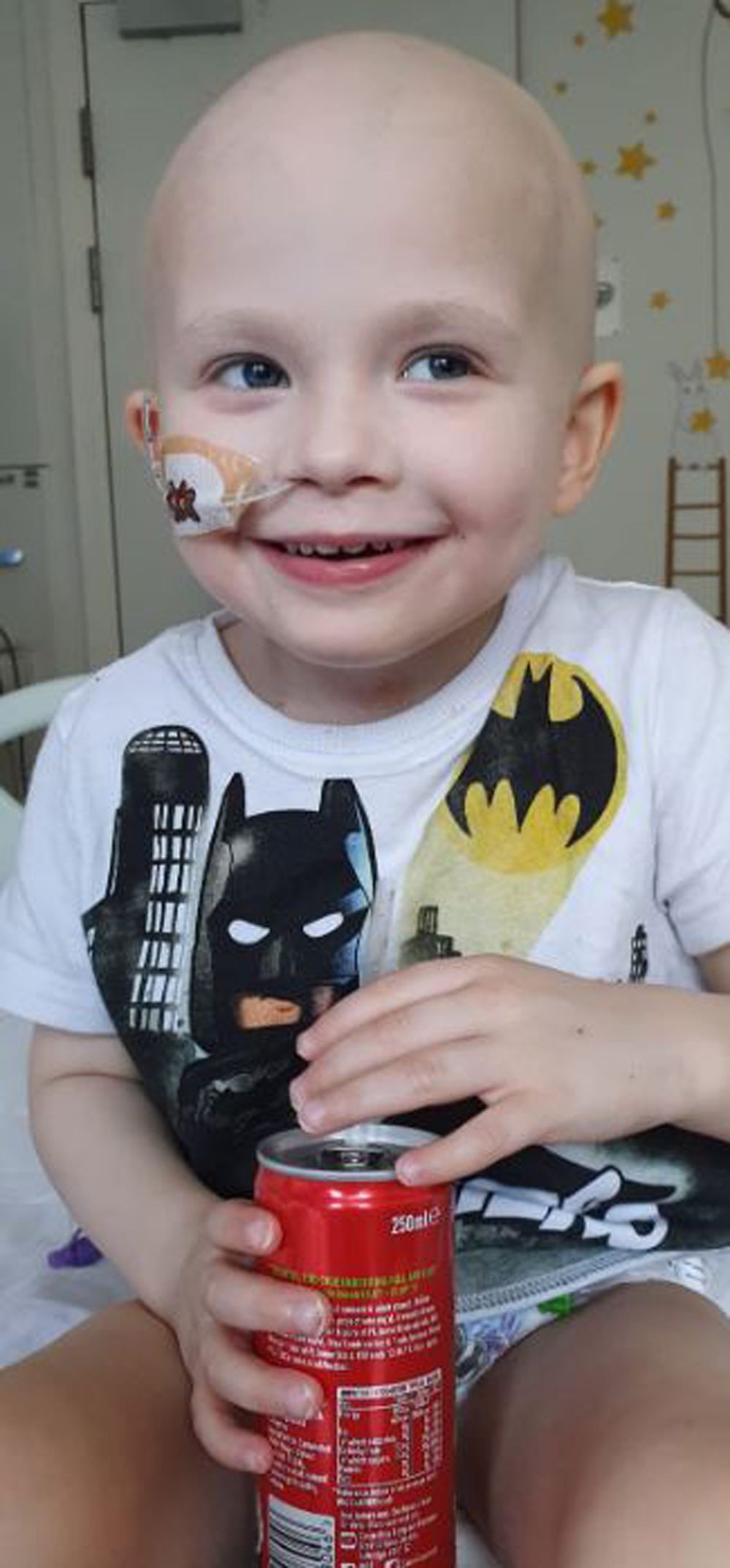
She continued:
“He's full of energy around the clock now – not just for a few days a month."
“I don't think we realized just how poorly he had been for the last four years until he recovered. That had become our normal."
Taken off immunosuppressants in May 2020, a month later, blood tests revealed that Henry had the blood count of an average four-year-old.
“For his whole life he's been in and out of hospital and now, finally, he can start to live like any other kid," said Zoe.
“Ringing the end of treatment bell was such a big deal for all of us."
“It felt like the end of that chapter in our lives."
Desperate to raise awareness of DBA and the importance of bone marrow donation, Zoe now has an important message she wants to send to whoever saved her son's life.
“We're so grateful to whoever it was that donated their bone marrow for Henry," she said.
“To anyone else out there who isn't on the donor register, please sign up."

She continued:
“All it takes is a bit of your spit sent in the post and it could quite literally save someone's life."
To find out more about registering as a bone marrow donor, click here.







 @KBN/Instagram
@KBN/Instagram 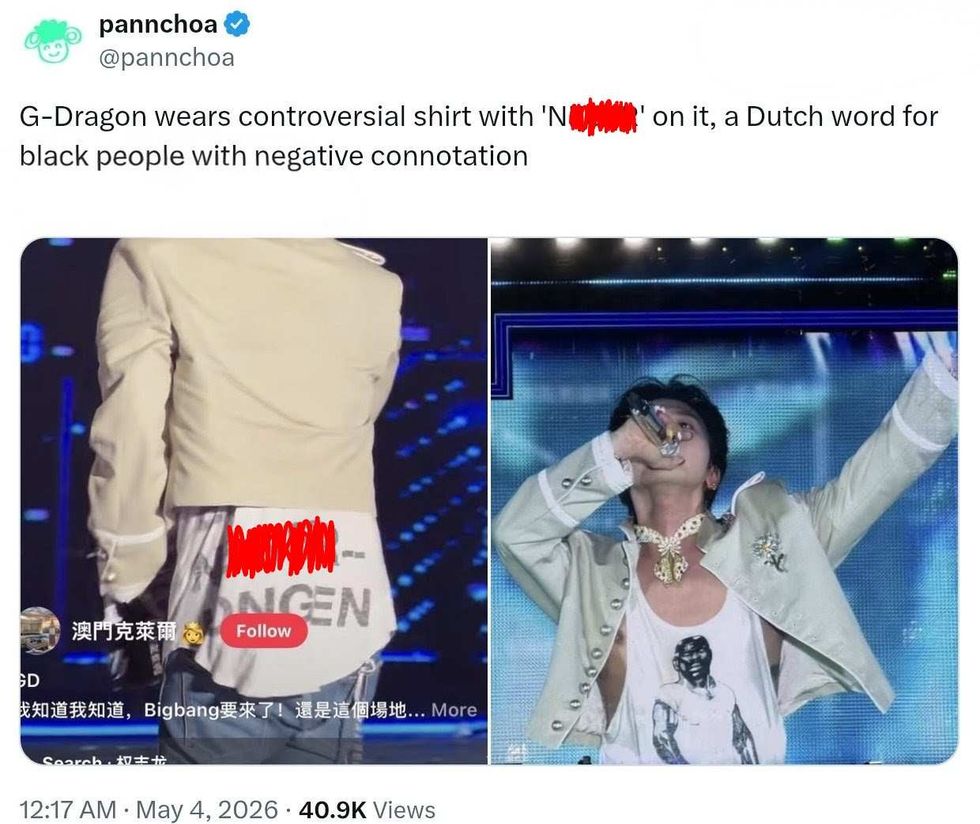 @pannchoa/X
@pannchoa/X @KFloopNet/X
@KFloopNet/X @KFloopNet/X
@KFloopNet/X @KFloopNet/X
@KFloopNet/X @KpopInsider/X
@KpopInsider/X reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram
 reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram @hh.azzy/Instagram
@hh.azzy/Instagram reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram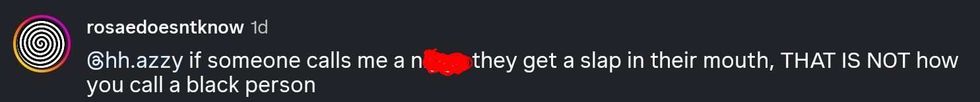 reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram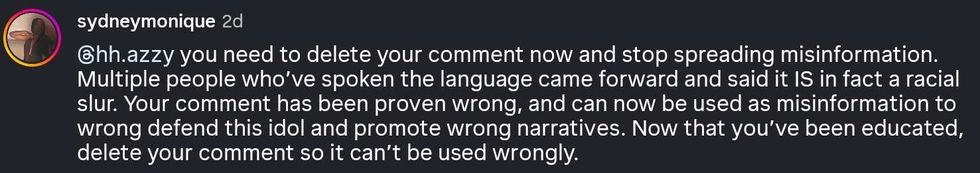 reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram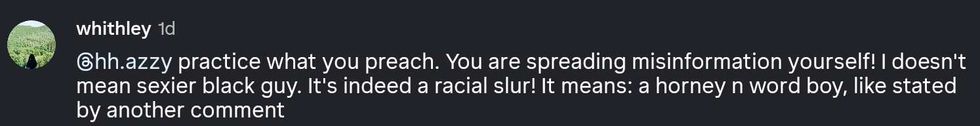 reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram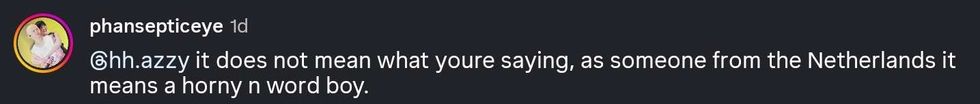 reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram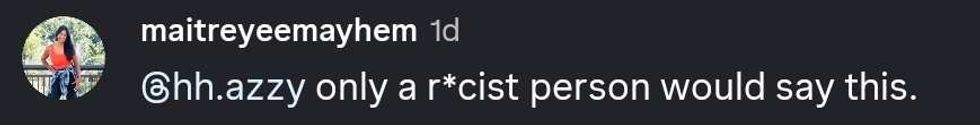 reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram reply to @hh.azzy/Instagram
reply to @hh.azzy/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram reply to @xxxibgdrgn/Instagram
reply to @xxxibgdrgn/Instagram






 @realDonaldTrump/Truth Social
@realDonaldTrump/Truth Social
 @WhiteHouse/X
@WhiteHouse/X