A mom-of-two diagnosed with ovarian cancer more than four decades after the organs were removed during a full hysterectomy has expressed her zest for life almost four years after doctors warned that she may not live to see Christmas.
Now 71, retired nursery nurse Janet Harvey was just 27 when she had a full hysterectomy to remove her womb, cervix, fallopian tubes, and ovaries after battling heavy periods and agonizing cramps.
So, years later, when she experienced bloating, abdominal pain, and diarrhea, eventually leading to a diagnosis of ovarian cancer in February 2016 – 41 years after her operation – she was flabbergasted.

Doctors explained to Janet, of Portsmouth, Hampshire, England, who has two children, Dawn, 50, who works in travel, and Anthony, 48, a naval base guard, with her ex-Royal Marine husband Paul, 74, that a tiny smattering of ovarian cells remained after the surgery and, in time, had become cancerous.
As the cancer – classed as stage three – had also spread to her peritoneum, which forms part of the abdominal lining, Janet said her prognosis was grave, adding: “Everybody thought me getting ovarian cancer when I no longer had ovaries was impossible. But it turns out that, after my hysterectomy, some ovarian cells had remained.
“I was diagnosed in February 2016 and when I asked how long I had, I was told, 'Don't make plans for Christmas.' But I begged doctors to give me a chance to fight. I didn't ask for this and I wanted to buy some time and some hope."
She added: “I promised my family I'd fight it with every ounce of strength I had and that's what I did. Now, almost four years on, I do feel like I've stuck two fingers up to cancer."
After having children, Janet, who also has grandchildren, developed a string of nasty symptoms, including heavy periods and pain during intercourse and, after other treatments failed, in 1975 she had a full hysterectomy, which plunged her into menopause at the age of just 27.
“The pain and cramps were immediately better, but I soon started to suffer with night sweats, which the doctor at a post-op check-up said were because of the menopause," she recalled.

Waking up soaked in sweat and sometimes having to change her sheets in the night, Janet was prescribed hormone replacement therapy, initially in pill form and then in her 40s as an estrogen gel, after the sweating returned.
Hoping her health problems were behind her, Janet was shocked when, in around 2006, she was hit by a wave of new complaints.
“I started getting bloating and diarrhea and saw the doctor, who thought it was irritable bowel syndrome and prescribed some medication," she said.
“That worked at first but, over the years, I had to keep upping my dosage, but the symptoms would soon return. "
Disaster then struck in 2013 during a trip to the French capital, Paris, with her daughter Dawn and granddaughter, who was celebrating her 18th birthday.
She recalled: “I had an accident and lost control of my bowels when we were walking down the Champs-Élysées. I was wearing white jeans, which made it even worse. Dawn had to give me her jumper to tie around my waist.
“Not only did it happen in front of everyone on a busy street, but it happened in front of my granddaughter."

Forced to clean up in a public toilet while her daughter bought her a change of clothes, Janet was devastated by what happened.
She said: “It was so humiliating. I knew in that moment that something was wrong and that I had to go back to the doctor in the UK."
Referred for tests at Southampton General Hospital, including a colonoscopy – where a long, thin tube with a small camera inside it is used to examine the bowels – Janet's results were clear.
So, in November 2013, she had a pacemaker-like device called a sacral nerve stimulator, which uses a low-voltage electrical current to send impulses to the nerves controlling the bowels, surgically implanted into her hip.
“Afterwards, my bowel control was much better," said Janet. “The bloating and abdominal pain was still sometimes there, but I kept telling myself that it was just a machine and it wasn't going to solve everything.
“Being 90 percent better still put me in a much more positive place than I had been."
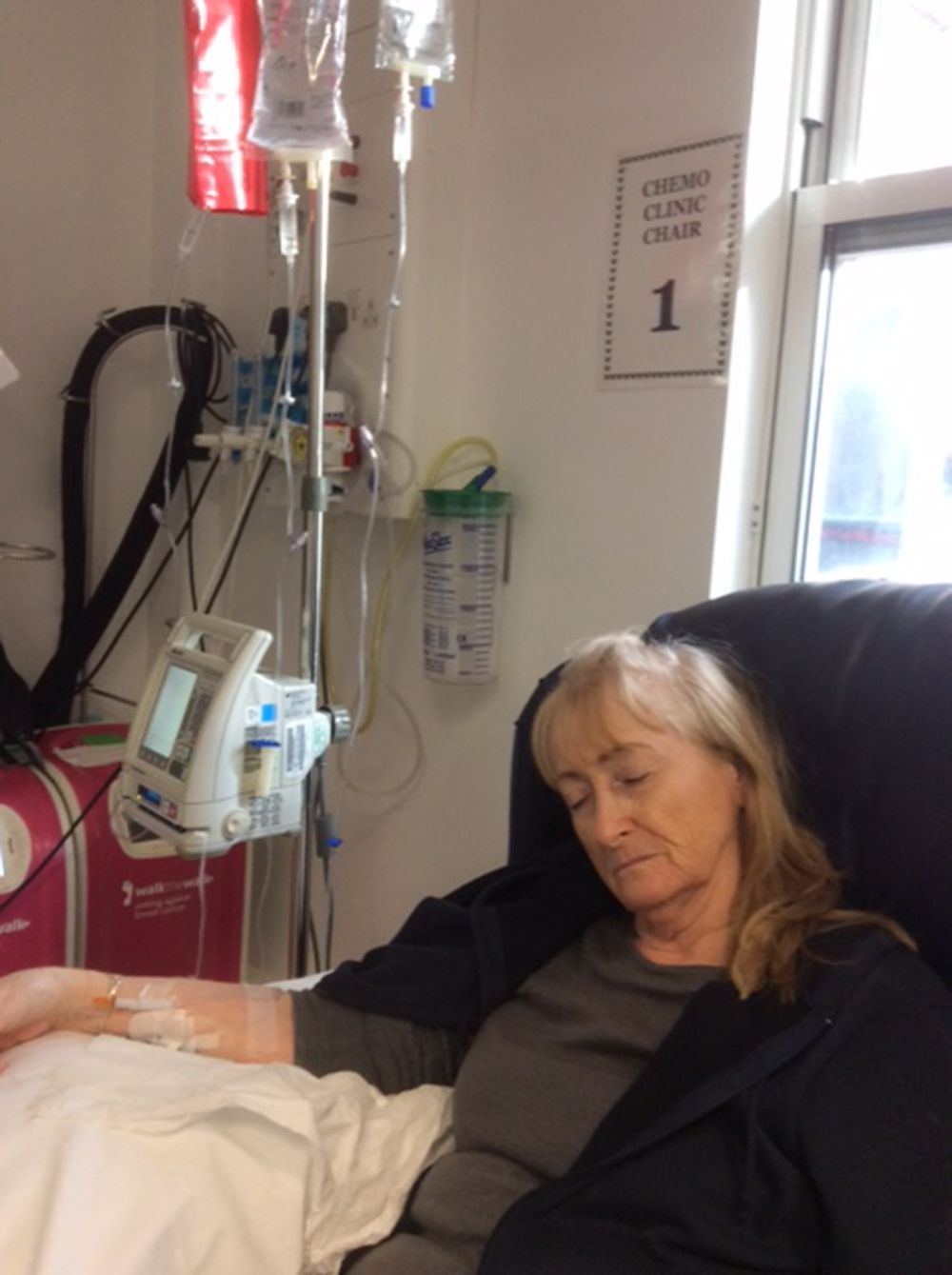
Then, in late 2015, Janet had a nasty fall in a beauty salon, leading to her running a hot bath later to ease her aches and pains, when her husband spotted something that changed her life forever.
She said: “I was in so much pain that Paul was helping me into the bath and he suddenly said, 'Look at your backside.' It turned out my skin was black with an enormous bruise."
Worried she had done herself some real damage, she saw her GP, who sent her back to Southampton Hospital.
According to Harvard Medical School, easy bruising like Janet's following her fall can be symptomatic of some cancers, due to the low platelet count in patients' blood – and, while her X-rays were clear, doctors realized something sinister was going on.
“I started to have all sorts of other tests, including another colonoscopy," she said. “Doctors told me they thought I was dealing with some form of cancer, but weren't sure where it was coming from."
In January 2016, Janet had a full body scan, which showed two worrying masses where her ovaries once were.

“Those results were indicating something we had all thought was impossible – that I had ovarian cancer, but no ovaries," she said. “My results were sent to specialists around the world to look at, who confirmed in February 2016 that I did indeed have ovarian cancer.
“The way they explained it to me was that my ovaries had been too big for my fallopian tubes, so whenever they were cramping and contracting, cells were almost being shaved off the sides.
“Then, when I had my hysterectomy, some ovarian cells remained, which is rare, but can happen. Normally, those cells would naturally break down, but in my case, they developed cancer."
A more targeted scan and a biopsy showed that Janet had two tumors, as well as cancer cells being evident in her abdominal lining, meaning the disease was classed as stage three and her only treatment option was aggressive chemotherapy.
Despite being warned of difficult side effects, determined to keep fighting, she broke the bombshell news to her family and agreed to proceed with chemo.
She continued: “I gathered everybody at my house – luckily my children both live within walking distance – and told them all to hold hands, so that I could have the strength to say what I needed to. I started to cry, and Paul offered to tell them instead, but the news had to come from me."
Janet added: “I told them I had cancer, and that I didn't know if I was still going to be here at Christmas, but that I'd fight it with all I had. I wasn't ready to go, I still had so much I wanted to do with my life."
Two weeks later, Janet began chemotherapy – the first of six rounds. And in April 2016, just before her second session, she was also given a place on a trial for a targeted therapy drug called bevacizumab – known by the brand name Avastin.
Given in combination with chemotherapy through a drip, according to the charity Target Ovarian Cancer, it aims to interfere with the cancer's growth by targeting a protein on the cell surface, which usually helps to develop a blood supply. As a result, the oxygen and nutrient supplies are reduced, thus, hopefully, shrinking or stopping the tumor from growing.

“Some people said a trial was risky and that I could die, but doctors had told me not to make plans for Christmas, so I could die if I did nothing," said Janet, who also hoped that being a guinea pig would help to progress treatment for the disease.
And, still receiving her combined treatment almost four years on, although her cancer is still classed as stage three, neither tumor has grown.
Janet, whose progress is monitored by blood tests every nine weeks, is feeling positive and, since 2017, has worked closely with Target Ovarian Cancer to raise awareness, after asking her loved ones make a donation to them in lieu of presents for her 50th wedding anniversary.
Keen for women to take note of symptoms like persistent bloating, loss of appetite, pelvic or abdominal pain, changes in bowel habit, needing to wee more urgently or more often, extreme fatigue, and unexplained weight loss, she said: “Target Ovarian Cancer have been a fantastic support. Now I really hope that reading my story will help others out there to take note of these symptoms before it's too late.
“Nobody knows when their time is and I feel so lucky to still be here almost four years on.
“I think of people as being born with a deck of cards. Every day of your life, a new one is turned over and you have to deal with whatever that card brings.
“I may have been given the cancer card, but it doesn't mean it has to take over my life."

Rebecca Rennison, Director of Public Affairs and Services at Target Ovarian Cancer, said: “Removal of the ovaries and fallopian tubes greatly reduces the risk of ovarian cancer, and is a key preventative surgery for women who are at higher risk of ovarian cancer, for example due to an inherited genetic mutation.
“However, a very small risk of developing ovarian cancer can remain. Ovarian cancer is used to describe a range of cancers which originate in or around the ovaries, meaning removal of the ovaries alone does not completely remove the risk of developing the disease."
Target Ovarian Cancer is the UK's leading ovarian cancer charity. Anyone worried about ovarian cancer can contact their nurse-led Support Line at targetovariancancer.org.uk/supportline or call 020 7923 5475.



















 @realDonaldTrump/Truth Social
@realDonaldTrump/Truth Social @aricchen/X
@aricchen/X @realDonaldTrump/Truth Social
@realDonaldTrump/Truth Social @hydemia411/Bluesky
@hydemia411/Bluesky

